© 2024 Dott. Scotti Fabrizio - P.IVA 03393000967
A cataract is a cloudy film over the lens of your eye that adversely affects your vision. Cataracts are typically a result of aging, and they’re more common in the elderly. According to the National Eye Institute, by the age of 80, more than half of all Americans have cataracts or have been treated surgically for cataracts.
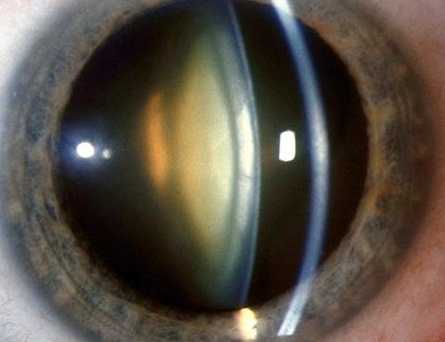

Cataracts aren’t contagious, and they can’t travel from one eye to the other. But cataracts may occur in one eye or both eyes independently. While most cataracts are brought on by aging, some types aren’t. These include:

The symptoms most people experience with cataracts are:
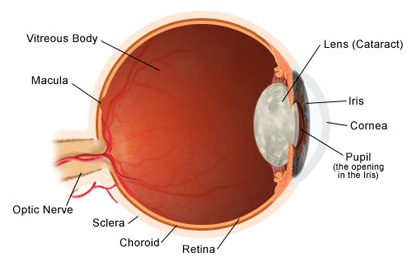
Cataracts form on the lens of your eye, which is directly behind the iris and the pupil. The lens works like a camera lens, focusing light on the retina in the back of your eye, which then forms an image for your brain. The lens, comprised of water and protein that allows light to pass through while keeping the lens clear, enables you to see far away and close up clearly.
As you age, these proteins clump together, making that part of the lens thicker — which causes blurry vision. This clumping of proteins is what is called a cataract. It can grow larger over time, obscuring more of the lens and making it more difficult to see.
Aside from aging, researchers have discovered other potential causes of cataracts, such as diabetes, alcohol abuse and smoking. The primary cause of cataracts is simply that the proteins in the lens change from wear and tear on the eye over decades.
Age-related cataracts are by far the most common type. Cataracts that develop from old age can affect your vision in two ways:
When the color-changing effect is present, your lens slowly darkens with time. It typically appears as a yellowish tint and grows to more of a brownish shade over a period of years. Initially, the light tinting may not be a problem for you, but it eventually affects the amount of light and sharpness of the image projected onto your retina. Advanced discoloration limits your ability to identify the difference between purples and blues.
Cataracts can be detected through routine eye exams. Typically, they’re discovered in the following types of tests at your eye doctor’s office:
Early cataract formation can be dealt with by improving your vision with anti-glare sunglasses, new eyeglasses, magnifying lenses and brighter lighting. If the cataracts have advanced to the degree where these measures aren’t effective, then CATARACT SURGERY is the only remaining treatment.
In surgery, either the cataract itself is removed or your entire lens is removed and then replaced with an artificial lens. A cataract’s removed only if the vision loss interferes with daily activities like reading, driving or watching TV. Consult your eye doctor about surgical options and whether it’s a good choice for you. Since postponing cataract surgery doesn’t cause long-term eye damage or make the surgery more difficult, there’s no rush to receive surgical treatment.
There are occasions where your ophthalmologist may recommend removing a cataract surgically even if it’s not causing problems with your vision. For example, a cataract needs to be removed if it prohibits the treatment or examination of another eye issue, such as siabetic retinmopathy or macular degeneration.
If you’re concerned about the safety and effectiveness of cataract surgery, don’t be. It’s one of the most effective and safest forms of surgery. Cataract removal is one of the most common surgical procedures in the United States, and in 90 percent of cases, according to a 2015 report by the National Eye Institute, patients report improved vision after the surgery.
There are risks with any surgery, however, regardless of the procedure. Common risks include bleeding and infection. Prior to your surgery, you may be asked to stop taking some medications that could increase the risk of bleeding during the surgery. After the surgery, you’ll have to be diligent in maintaining cleanliness in your eye to prevent infection. This includes washing your hands before touching your eye, and taking prescription drugs to reduce the chance of infection. Infection is a serious matter as it may result in a loss of vision.

